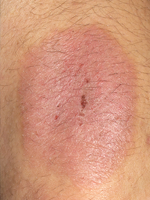
A novel compound currently in development, ivermectin 1% cream, targets the underlying cause of papulopustular rosacea (a prevalent type of rosacea), which is associated with an infestation of Demodex folliculorum, a skin mite that harbors the bacteria linked to rosacea. The current understanding is that infestation of the Demodex microorganisms triggers a complex cascade of events that produce the symptoms of rosacea. In a pair of phase 3 clinical trials, ivermectin has been shown to clear the papules and pustules characteristic of papulopustular rosacea. The results were recently published in the Journal of Drugs in Dermatology (Stein Gold LF, et al. J Drugs Dermatol. 2014;13:316-323), and were also presented at the 2014 American Academy of Dermatology (AAD) meeting.
Applied once daily to the face of patients with moderate-to-severe papulopustular rosacea, ivermectin 1% cream effectively met the studies’ 2 primary end points—clearing the patients’ skin of papules, pustules, and persistent erythema, and reducing the number of these inflammatory lesions.
Discussing the results associated with ivermectin 1% cream, senior investigator of 1 of the 2 studies, Zoe D. Draelos, MD, Consulting Professor in the Department of Dermatology at Duke University School of Medicine, NC, told American Health & Drug Benefits, “The study showed high efficacy for inflammatory rosacea, with an excellent safety profile.”
Rationale for Ivermectin
Papulopustular rosacea is characterized by facial papules, pustules, and persistent erythema. Multiple factors are believed to cause rosacea, including the presence of inflammatory infiltrates in the skin, a heightened immune response, exogenous factors (eg, ultraviolet light, heat, alcohol). Infestation with the skin mite D folliculorum is implicated in the development of the papules, pustules, and chronic erythema that are the hallmark of papulopustular rosacea. These factors can activate neurovascular and immune responses resulting in inflammation and erythema that produces the flares of rosacea. By reducing the Demodex mite count, this novel medication can address the underlying cause of papulopustular rosacea.
Ivermectin 1% cream is antiparasitic against the parasite D folliculorum, as well as anti-inflammatory, providing a novel treatment option with a new mechanism of action for patients with rosacea.
Ivermectin is currently under review by the US Food and Drug Administration for the treatment of rosacea. If approved, it will be the first and only topical product that specifically addresses this underlying cause of the skin disorder.
Design of 2 Phase 3 Multicenter Trials
The 2 studies compared ivermectin 1% cream with a control vehicle cream in a total of 1371 patients (combined) with moderate-to-severe rosacea (683 patients in Study 1 and 688 patients in Study 2). The designs were identical; each study was a double-blind, parallel-group, 12-week clinical trial in which patients were randomized in a 2:1 ratio to receive ivermectin or a control cream.
The 2 coprimary end points were the percentage of patients who achieved a score of “clear” (ie, no inflammatory lesions, no erythema) or “almost clear” (very few small papules/pustules, very mild erythema) on the Investigator’s Global Assessment (IGA) scale at week 12, and the percentage change in inflammatory lesion count from baseline to week 12. Other measurements included the patients’ evaluation of improvement of their rosacea at the end of the study compared with their condition at baseline, as well as several quality-of-life measures. The drug’s safety was also assessed.
The patients’ mean age was 50 years, approximately 96% were white, and approximately 67% were women. Patients had an average of 32 lesions, with more than 75% of patients classified as having moderate rosacea and approximately 21% considered to have severe rosacea. More than 91% of patients completed the studies in all arms.
Ivermectin Cleared Skin Lesions
Assessments at week 12 in both trials showed that a significantly higher percentage of patients receiving ivermectin 1% cream achieved treatment success by IGA scale. The proportion of patients deemed “clear” or “almost clear” of lesions at week 12 for studies 1 and 2 were 38.4% and 40.1%, respectively, with ivermectin compared with 11.6% and 18.8%, respectively, for the vehicle (both P <.001). The differences between the arms became apparent by week 4.
The reduction in inflammatory lesion counts was also greater in the active treatment arms. The average patient receiving ivermectin exhibited 8 fewer lesions than patients receiving the vehicle (P <.001), which amounted to an approximate 75% reduction in lesion counts with ivermectin and a 50% reduction with the vehicle cream.
Whereas approximately 50% of the patients in all of the arms reported cutaneous symptoms before the start of the study, especially mild or moderate dry skin or pruritus, the majority of patients reported none of these symptoms after treatment.
The investigators concluded in their article, “These results are particularly robust when considering the stringent inclusion criteria…and outcome assessments. At week 12, IVM [ivermectin] 1% showed a treatment effect that was highly significant (P <.001) in all primary and secondary endpoints, with greater efficacy observed by week 4 in each study.”
High Ratings by Patients
The patients themselves also rated their degree of improvement after treatment. The result was considered “excellent” or “good” in 69% and 66.2% of patients in the ivermectin arms compared with 38.6% and 34.4% of patients in the vehicle arms (P <.001). “Excellent” improvement was reported by 34.3% and 32% of patients receiving ivermectin versus 9.5% and 7.3% of patients who received the control treatment.
Patients receiving ivermectin also had improved quality-of-life scores, and at the end of each study, more patients in the ivermectin groups (53%) than the vehicle groups (35%) considered their disease to have no effect on their overall quality of life (P <.001).
Safety Established
Ivermectin 1% cream was deemed safe and tolerable in both studies. The most common treatment-related side effect in Study 1 was the sensation of skin burning (1.8% with ivermectin, 2.6% with the vehicle), and in Study 2 it was pruritus and dry skin (0.7% and 0.9%, respectively). No clinically significant abnormalities were demonstrated by laboratory tests.
“This drug was exceptionally well tolerated, very safe, as well as efficacious,” said lead investigator Linda F. Stein Gold, MD, Director of Dermatology Research at Henry Ford Medical Center, Detroit, MI, who presented the results of the studies at the AAD meeting.