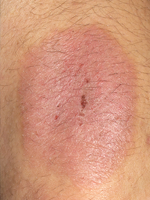
The pathogenesis of rosacea—a chronic inflammatory disorder that is characterized by facial papules, pustules, and persistent erythema—is multifactorial. Many factors are believed to activate neurovascular and immune responses, leading to inflammation that results in “flares.” One of these components is believed to be infestation with the microorganisms Demodex folliculorum and Demodex brevis, which are skin mites.
A therapeutic compound, ivermectin 1% cream, which is currently under review by the US Food and Drug Administration, is the first to target this underlying cause of rosacea. In clinical trials, ivermectin 1% cream proved effective for the rosacea subtype called papulopustular rosacea, significantly improving the odds of treatment success versus control treatment.1
Papulopustular rosacea is the second most common subtype of rosacea.2 It is characterized by persistent central facial erythema with transient, central facial papules or pustules, or both. These symptoms are the result of chronic inflammation.2
Slightly more common is the subtype of erythematotelangiectatic rosacea, marked by prolonged flushing of the skin that can be triggered by stress, hot or spicy foods, alcohol, hot showers, sun exposure, and extreme temperatures. Less common subtypes are phymatous rosacea, in which skin (usually involving the nose) becomes thickened, and ocular rosacea, the symptoms of which include a variety of unpleasant sensations within the eyes.2
An Unmet Medical Need
Topical azelaic acid and metronidazole are effective for many people with moderate-to-severe papulopustular rosacea3; however, not all patients respond to these traditional agents. A national survey of persons with rosacea showed that almost 50% switched medications because of a lack of improvement,4 underscoring the need for treatments with new mechanisms of action.
Because of the underlying role of inflammation, most current therapies aim to modulate various factors along the inflammatory cascade. For example, low-dose doxycycline is an anti-inflammatory agent that is often effective in the papulopustular rosacea subtype when topical treatments are insufficient. For the erythematotelangiectatic subtype, brimonidine tartrate addresses the vascular abnormality that produces erythema.
The exact role of Demodex in causing rosacea is not well understood, but it is believed that the mites—or the Bacillus oleronius bacteria that they harbor—trigger inflammatory or immune reactions that result in the symptoms of rosacea.5,6 Ivermectin 1% cream has a unique mechanism of action among current treatments for rosacea; unlike available treatments, this unique mechanism addresses the inflammatory process involved in rosacea and the key organism, Demodex. Current standard-of-care agents are believed to work by inhibiting the reactive oxygen species caused by neutrophils, by combating bacteria in the skin, and by generally reducing inflammation, but they do nothing to eradicate Demodex.7
Effect of Demodex in the Skin
Demodex mites are often found in the skin of healthy individuals. The mere presence of these organisms, therefore, is not sufficient to cause rosacea, but the overproliferation of Demodex could be. The mean density of the mites in the skin of patients with rosacea has been shown to be more than 10 times higher than among individuals without rosacea, and even greater in patients with the papulopustular rosacea subtype.8 In one study of rosacea, Demodex was identified in the follicle secretions of 90% of 92 patients with papulopustular rosacea compared with only 12% of the 92 controls.9 The hypothesis is that in individuals with papulopustular rosacea, these mites breach the skin barrier, penetrate into follicles, induce a hypersensitivity reaction, and produce skin lesions.6
Other research points to the role of Demodex as a vector for B oleronius. It is hypothesized that through various processes, it is the presence of the bacteria that leads to tissue degradation, the production of antigens, the stimulation of a strong inflammatory response and production, or the exacerbation of skin lesions.6
In summing up the potential role of Demodex in inducing rosacea, Jarmuda and colleagues concluded that “immunological conditions favour the development of different types of micro-organisms, including Demodex mites. Other characteristic features of rosacea patients, such as increased vascularization and elevated temperature, may further promote the growth of the organisms. Developing Demodex mites may be causative agents of rosacea through various mechanisms: they may mechanically block hair follicles, secrete digestive enzymes, destroy the epithelial barrier or trigger reactions of the immune system.”6
How Ivermectin Works
Ivermectin is not an antibiotic. It is a member of the avermectin class of compounds. These drugs, which have been used in agriculture and in veterinary medicine for years, exert anti-inflammatory effects in several ways: they inhibit lipopolysaccharide-induced inflammatory cytokines, such as tumor necrosis factor alpha and interleukin (IL)-1b, and they upregulate the anti-inflammatory cytokine IL-10.10,11
In addition to working via an anti-inflammatory mode of action, ivermectin also exerts antiparasitic effects. It acts as an agonist (ie, it activates) of the GABA neurotransmitter in the nerve cells of Demodex. It also binds to glutamate-gated chloride channels in nerve and muscle cells.12 This is the way ivermectin blocks the transmission of nerve signals of the mites and is able to paralyze and kill these organisms.12
This mechanism of action may be responsible for the efficacy that ivermectin has already shown in clinical trials in reducing Demodex mites in cutaneous demodicidosis (obvious Demodex facial infestation)13 and blepharitis (inflammation of the eyelid).14 It has also proved effective in the treatment of scabies (infection with the Sarcoptes scabiei mite)15 and head lice.16
In the recent publication of phase 3 trial results with ivermectin, Stein Gold and colleagues noted, “Medications with both anti-inflammatory and anti-parasitic activity have not yet been developed for rosacea treatment. Accordingly, ivermectin 1% cream is an innovative therapy addressing these relevant pathogenic factors in PPR [papulopustular rosacea] and is a novel option for treatment of this condition.”1
References
- Stein Gold L, Kircik L, Fowler J, et al; for the Ivermectin Phase III Study Group. Efficacy and safety of ivermectin 1% cream in treatment of papulopustular rosacea: results of two randomized, double-blind, vehicle-controlled pivotal studies. J Drugs Dermatol. 2014;13:316-323.
- Wilkin J, Dahl M, Detmar M, et al. Standard classification of rosacea: Report of the National Rosacea Society Expert Committee on the Classification and Staging of Rosacea. J Am Acad Dermatol. 2002;46:584-587.
- van Zuuren EJ, Kramer SF, Carter BR, et al. Effective and evidence-based management strategies for rosacea: summary of a Cochrane systematic review. Br J Dermatol. 2011;165:760-781.
- Elewski BE. Results of a national rosacea patient survey: common issues that concern rosacea sufferers. J Drugs Dermatol. 2009;8:120-123.
- Szkaradkiewicz A, Chudzicka-Strugała I, Karpiński TM, et al. Bacillus oleronius and Demodex mite infestation in patients with chronic blepharitis. Clin Microbiol Infect. 2012;18:1020-1025.
- Jarmuda S, O’Reilly N, Żaba R, et al. Potential role of Demodex mites and bacteria in the induction of rosacea. J Med Microbiol. 2012;61(pt 11):1504-1510.
- Del Rosso JQ, Gallo RL, Kircik L, et al. Why is rosacea considered to be an inflammatory disorder? The primary role, clinical relevance, and therapeutic correlations of abnormal innate immune response in rosacea-prone skin. J Drugs Dermatol. 2012;11:694-700.
- Forton F, Seys B. Density of Demodex folliculorum in rosacea: a case-control study using standardized skin-surface biopsy. Br J Dermatol. 1993;128:650-659.
- Georgala S, Katoulis AC, Kylafis GD, et al. Increased density of Demodex folliculorum and evidence of delayed hypersensitivity reaction in subjects with papulopustular rosacea. J Eur Acad Dermatol Venereol. 2001;15:441-444.
- Ci X, Li H, Yu Q, et al. Avermectin exerts anti-inflammatory effect by downregulating the nuclear transcription factor kappa-B and mitogen-activated protein kinase activation pathway. Fundam Clin Pharmacol. 2009;23:449-455.
- Zhang X, Song Y, Ci X, et al. Ivermectin inhibits LPS-induced production of inflammatory cytokines and improves LPS-induced survival in mice. Inflamm Res. 2008;57:524-529.
- Junquera P. Ivermectin: safety summary for veterinary use on dogs, cats, cattle, sheep, goats, swine and poultry. Poisoning, intoxication, overdose, antidote. Parasitipedia.net. Updated August 3, 2014. http://parasitipedia.net/index.php?option=com_content&view=article&id=2344&Itemid=2996. Accessed August 7, 2014.
- Forstinger C, Kittler H, Binder M. Treatment of rosacea-like demodicidosis with oral ivermectin and topical permethrin cream. J Am Acad Dermatol. 1999;41(5 pt 1):775-777.
- Holzchuh FG, Hida RY, Moscovici BK, et al. Clinical treatment of ocular Demodex folliculorum by systemic ivermectin. Am J Ophthalmol. 2011;151:1030-1034.
- Trendelenburg M, Büchner S, Passweg J, et al. Disseminated scabies evolving in a patient undergoing induction chemotherapy for acute myeloblastic leukaemia. Ann Hematol. 2001;80:116-118.
- Pariser DM, Meinking TL, Bell M, Ryan WG. Topical 0.5% ivermectin lotion for treatment of head lice. N Engl J Med. 2012;367:1687-1693.